There’s No “Best” Rehab Exercise - Only the Right One For You
If you’ve ever had an injury, you’ve probably been given a list of exercises to do to help you recover. Or maybe you’ve searched for exercises online and found a handful of the “best” or “number 1” exercise for your injury. The problem is that even good exercises don’t work if they don’t fit into your life. That’s where most rehab plans fall apart. It’s easy to get caught up trying to find the perfect exercise, but the reality is the best exercise is the one that actually works for you. Many people don’t fail rehab because the exercises are wrong or because they lack motivation. They fail because the plan doesn’t stick.
If you’ve ever had an injury, you’ve probably been given a list of exercises to do to help you recover. Or maybe you’ve searched for exercises online and found a handful of the “best” or “number 1” exercise for your injury. The problem is that even good exercises don’t work if they don’t fit into your life. That’s where most rehab plans fall apart. It’s easy to get caught up trying to find the perfect exercise, but the reality is the best exercise is the one that actually works for you. Many people don’t fail rehab because the exercises are wrong or because they lack motivation. They fail because the plan doesn’t stick.
Why There’s No “Best” Rehab Exercise
There is no universal “best” rehab exercise. The same exercise that works well for one person might feel frustrating, confusing, or unrealistic for someone else. This is because not only do injuries differ, but because people differ as well. Your time, experience, goals, and day-to-day life all shape what will actually work for you. Research often shows that different exercise approaches lead to similar outcomes. This tells us something important: there usually isn’t just one right way to rehab an injury. You have more good options than you think.
Why “Perfect” Exercises Often Don’t Work
That “perfect” exercise you saw online might not work for you because:
It’s too much for where you’re at right now.
It takes longer to set up or complete than you have time for.
It needs equipment you don’t have.
It looks impressive, but doesn’t actually relate to what you need.
What Makes a Rehab Exercise Actually Work
But here’s the important part: any exercise can be the right one for you, if it fits. An exercise is more likely to work when it:
Fits your life. You have the time, space, and equipment to actually do it consistently.
Makes sense to you. You understand what you’re doing and why you’re doing it.
Can be adjusted. It can be progressed, regressed, or modified depending on how you’re feeling.
Builds confidence. You feel like you’re moving forward, not second-guessing every rep.
The best exercise for you is one that checks these boxes. If an exercise misses even one of them, it becomes harder to stick with. We know from behaviour change research that people are more likely to stick with something when it feels manageable, it fits into their routine, and they understand why they’re doing it. Rehab is no different.
Why People Struggle to Stick With Rehab
This can be why people will bounce from exercise to exercise - not because nothing works, but because nothing works for them. It’s easy to find an exercise that’s touted as the solution to your pain, but if it doesn’t fit your situation, or you don’t feel like it’s helping you move forward, then it’s not the solution to your problem - and that’s okay.
The Real Goal of Rehab
There’s no perfect rehab exercise. Just one that fits your life, makes sense to you, and actually moves you forward. The more you realize there are multiple ways to get there, the easier it becomes to stop chasing the “best” exercise and start making real progress. The perfect exercise doesn’t exist in isolation - it only exists in the context of you. If the exercise doesn’t fit your life, it won’t fix your problem.
Why Your Arm Is Sore After Throwing (What’s Normal and When to Worry)
It’s common for baseball and softball players, especially pitchers, to experience arm soreness after throwing. Even when you’ve built up properly, your arm can still feel fatigued or achy after a game or bullpen session. This type of soreness is different from injury-related pain. It reflects the physical demands of throwing, not necessarily a problem. Understanding why your arm gets sore can help you manage it properly and recognize when something more serious might be going on.
It’s common for baseball and softball players, especially pitchers, to experience arm soreness after throwing. Even when you’ve built up properly, your arm can still feel fatigued or achy after a game or bullpen session. This type of soreness is different from injury-related pain. It reflects the physical demands of throwing, not necessarily a problem. Understanding why your arm gets sore can help you manage it properly and recognize when something more serious might be going on.
Why Throwing Is So Stressful on the Arm
Even with good mechanics, strength, conditioning and recovery, pitching is still stressful on the arm. This is due to the speed and forces generated during the throwing motion, particularly in the later phases. At ball release, the arm experiences a strong pulling (distractive) force, often exceeding body weight, that the shoulder muscles must control. Repeating this over the course of a game places a significant demand on the arm, even in well-conditioned athletes.
What Causes Arm Soreness After Throwing? (DOMS Explained)
Delayed onset muscle soreness is the stiffness and aching you feel after a new activity or a significant increase in workload. While we don’t fully understand it, the leading theory is that it results from small amounts of muscle damage and the body’s inflammatory response. Eccentric muscle actions, where muscles work to slow movement, are a major contributor. In throwing, the muscles of the shoulder girdle and arm work eccentrically to decelerate the arm after ball release. Over the course of an outing, this repeated demand can lead to soreness.
Does Lactic Acid Cause Arm Soreness?
Lactic acid is often blamed for muscle soreness, but this idea is outdated. Lactate (the correct term) does not cause the fatigue or burning sensation during activity, and it doesn’t explain soreness the next day. Lactate is cleared from the body relatively quickly. In pitching, the amount produced during a single throw is minimal and is typically cleared before the next pitch.
When Arm Soreness Is Normal (and When It’s Not)
It is normal for your shoulder and arm to be sore following pitching, and even into the next day. This is usually a general, fatigued soreness that improves within a day or two. Pay closer attention if you notice sharp or pinpoint pain, pain during throwing, loss of velocity or control, or soreness that continues to worsen over time. Soreness doesn’t mean something is wrong- it means your body was challenged, and this happens every time you step on the mound. But if that challenge exceeds what you’re prepared for, that’s when problems can develop.
Recovery Principles
There’s no magic cure for DOMS. The best approach is good, basic recovery: adequate sleep, nutrition and hydration, and appropriate spacing between throwing sessions. Lght physical activity can sometimes provide some temporary relief, but adding more work to an already fatigued arm usually just adds more stress. Recovery should support the system, not further stress it.
Some arm and shoulder soreness after throwing is completely normal. It reflects the high demands placed on the arm, even when you’re prepared well. Being sore isn’t a requirement for a good outing, and it’s not something to chase or avoid entirely. The key is understanding the difference between normal soreness and warning signs of overload. With proper training, recovery and monitoring, post-throwing soreness is simply part of the process, not a problem to fix.
Back Outside? Why Baseball Players Get Hurt Early in the Season (and How to Avoid It)
It’s that time of year again. The days are getting longer, the weather is improving, and baseball and softball teams across Ireland are starting to move from indoor sessions back outside. And with that comes a pretty common pattern. You’re throwing a bit harder, taking more swings, and running a bit more; it feels good to be back on a full field again. For the most part, nothing feels wrong in the moment. But then the next day, or a few sessions later, you start to notice a little bit of soreness, maybe something more specific, or something that lingers and starts to affect how you play. If that’s you, you haven’t done anything wrong, but your body is telling you something - it’s just not always obvious what.
It’s that time of year again. The days are getting longer, the weather is improving, and baseball and softball teams across Ireland are starting to move from indoor sessions back outside. And with that comes a pretty common pattern. You’re throwing a bit harder, taking more swings, and running a bit more; it feels good to be back on a full field again. For the most part, nothing feels wrong in the moment. But then the next day, or a few sessions later, you start to notice a little bit of soreness, maybe something more specific, or something that lingers and starts to affect how you play. If that’s you, you haven’t done anything wrong, but your body is telling you something - it’s just not always obvious what.
Why Injuries Happen Early in a Baseball Season
The start of the baseball and softball season is one of the most common times for injuries to show up. Even at the professional level, a large portion of injuries happen during spring training and early in the season. This is because the demands of the game change quickly. Indoor training has its place, but it comes with less space, lower intensity, and more controlled movement. When you move outside, everything ramps up at once - throwing distance increases, effort increases, volume often increases, and the overall unpredictability of the game comes back. Even if you’ve been training all winter, this is still a jump that happens all at once, and your body has to deal with all of it at the same time.
It’s Not Damage- It’s a Load Problem
A lot of these early-season issues get labelled as “overuse injuries”, which can make it sound like something is worn out or damaged. Most of the time, though, that is not what is happening. A better way to think about it is this: your body is dealing with a mismatch between what you’re asking of it and what it’s currently prepared for. Your body adapts to the loads you put through it, which is the purpose of training. However, these adaptations take time. When your throwing, hitting, and running all increase at once, your body just hasn’t caught up yet. It becomes a matter of “too much, too soon.”
Why This Happens Even If You Trained All Winter
It can be frustrating when you have been training consistently, doing some throwing and hitting, and still have something flare up. Even if you’ve been doing baseball activities indoors, it’s more about what you are preparing for. Indoor work doesn’t fully prepare you for full-distance throws, game-speed effort and repeated high-intensity movements. So when these show up all at once, the jump in demand can be enough to tip things over.
Soreness vs. Injury: What’s Normal?
Some soreness early in the season is completely normal. That general, slightly stiff feeling a day or two after training is just your body responding to something new. When talking about overuse injuries though, it tends to feel a bit different:
More specific to one area
More noticeable with certain movements
Sharper and/or more painful
Something that builds over a few sessions
Even with these symptoms, it still doesn’t necessarily mean a tissue is damaged. In a lot of cases, it’s better to think of this as a sensitive or irritated area, rather than a broken one.
How to Avoid the ‘Too Much, Too Soon’ Trap
This is where things get tricky, because no one is counting every throw or swing, and there is no perfect formula for how much is “too much.” But there are a few principles that go a long way:
You want to build, not spike. That means letting your throwing, hitting, and running increase gradually instead of all at once.
The point at which you’re starting to feel some soreness or fatigue in a body part is usually a good time to start to wind down from activities for that session. It’s usually better to nip things in the bud.
It’s tempting to go all out in those first few outdoor sessions, especially when you’re feeling good. But maxing out early is an easy way to create that mismatch between load and tolerance.
Early on, consistency matters more than intensity. Getting regular exposure to the demands of the game is what helps your body adapt.
Adding some basic strength work alongside your training can help build tolerance over time (especially if you’ve had issues in the past), but it doesn’t need to be complicated.
It’s worth expecting some soreness. Trying to avoid it completely usually leads to doing too little, which doesn’t help your preparation either.
What To Do If Pain Starts to Show Up
If you do start to notice something more specific or limiting, the goal isn’t to ignore it - but it’s also not to shut everything down. Most of the time, the best approach is to adjust your activity rather than stop it. That might look like reducing how much you’re throwing or hitting, lowering the intensity or modifying what you’re doing for a short period. From there, you can gradually build things back up once it settles. It’s a simple idea, but an important one: settle things down first, then build them back up. If it’s not settling or is starting to affect how you’re able to play, that’s usually a good time to get it checked out by someone who understands baseball and softball.
You’re Not Broken
The start of the season is always a bit of a shock to the system. More volume, more intensity, more effort, all at once. This is a really common part of the early season, even for players who have done a lot of things right leading into it. If something flares up, it doesn’t mean you’re fragile or injury-prone, or you’ve done something wrong. More often than not, it just means your body hasn’t caught up to what you’re asking of it yet, and it needs a bit more time to get there.
If you’re not sure how to balance training and recovery, or something starts to feel off, that’s exactly what I help with - especially for baseball and softball athletes navigating the start of the season.
What Is Evidence-Based Practice? A Better Way to Understand Research, Experience, and Patient Care
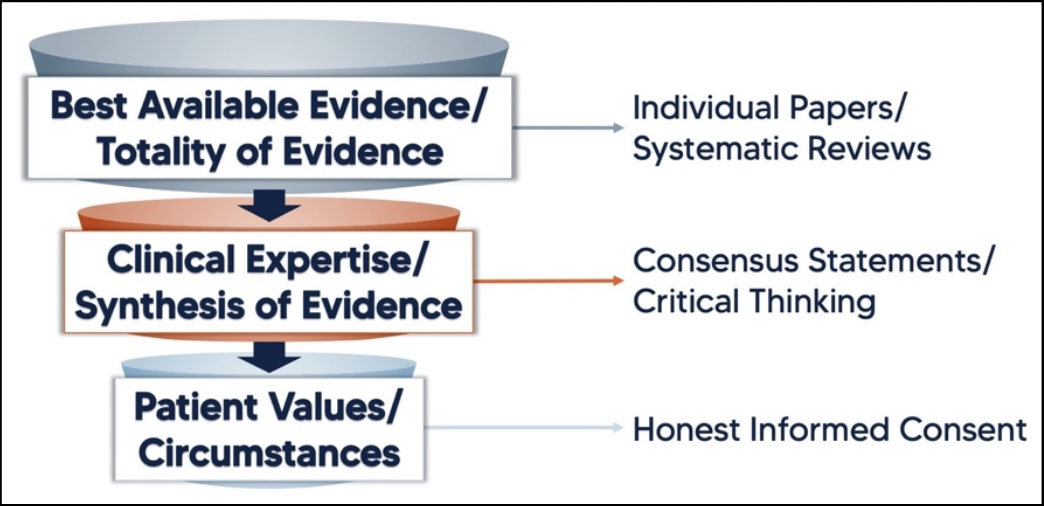
Evidence-based practice (EBP) is a term that gets used a lot in healthcare and rehab, but what does it actually mean? It’s often described as the integration of best available research, clinical expertise, and patient values. While all three are important, they aren’t truly equal or separate in practice. A more useful way to understand evidence-based practice is as a funnel — where research provides the starting point, clinical reasoning refines it, and the patient ultimately determines what is appropriate.
Evidence-based practice (EBP) is a term that gets used a lot in healthcare and rehab, but what does it actually mean? It’s often described as the integration of best available research, clinical expertise, and patient values. While all three are important, they aren’t truly equal or separate in practice. A more useful way to understand evidence-based practice is as a funnel — where research provides the starting point, clinical reasoning refines it, and the patient ultimately determines what is appropriate.
The scientific process is the best method we have for determining what is likely to be true. Researchers ask questions, test hypotheses, collect and analyze data, and repeat the process. Over time this builds a body of evidence that helps guide how we treat patients. Of course, research is not perfect. Studies can be flawed, data can be manipulated, and tightly controlled experiments may not always reflect real-world conditions. Still, when done well, scientific research provides the best starting point for understanding which treatments are most likely to work.
Clinical experience and observation are also forms of evidence, but they are considered lower levels of evidence because they are more susceptible to bias and lack experimental control. A patient may feel better after a treatment, but it can be difficult to determine whether that improvement was caused by the treatment itself or by other factors such as natural recovery or contextual effects. At the same time, clinical experience has value. Clinicians work with real patients who have unique circumstances, goals, and constraints that are often not represented in research studies.
“The literature cannot refute what is seen in the clinic, but it can refute our explanations of those experiences.”
The final piece of the puzzle is the patient. Ultimately, patients provide consent and decide whether a treatment plan fits their goals, beliefs, and circumstances.
This is where the funnel analogy becomes useful. At the top of the funnel is the best available research. Clinicians should start with the totality of evidence when deciding how to approach a condition. From there, that information is filtered through clinical expertise and practical experience. Finally, it narrows down to the individual patient, who determines whether the proposed treatment aligns with their preferences and circumstances.
Let’s look at an example.
A patient presents with Achilles tendon pain related to running and is diagnosed with a tendinopathy. Current research suggests that tendons respond well to progressive loading. Based on both research and clinical experience, the therapist recommends a heavy, slow calf raise program as the primary treatment. The patient agrees, and the plan moves forward.
But what if the patient is uncomfortable with that approach? Maybe they are inexperienced with resistance training, have had negative experiences lifting heavy weights, or simply prefer higher-repetition exercises. Instead of abandoning evidence-based practice, this is where the funnel becomes useful. We return to the top and reconsider the available options. While heavy, slow loading may be a preferred strategy in the literature, loading itself is the key stimulus for tendon recovery. Using clinical reasoning, the therapist might adjust the program to higher repetitions with lighter weight, or even begin with isometric exercises if symptoms are particularly irritable. These options may not be the exact approach used in research studies, but they still respect the underlying principles supported by evidence.
What if a patient requests a treatment that goes against the best available evidence? Evidence-based practice doesn’t mean ignoring the patient. Instead, it means having an honest discussion about the proposed treatment—its benefits, risks, and what the research actually shows. The clinician can then return to the top of the funnel, review the available options, and help the patient make an informed decision. Sometimes there is little or no research on a particular treatment. In those cases, if the risks are low and the patient understands the uncertainty involved, choosing to proceed can still fall within the spirit of evidence-based practice.
Evidence-based practice isn’t about blindly following research, relying solely on experience, or simply doing what the patient prefers. It’s about integrating all three — starting with the best available evidence, filtering it through clinical reasoning, and applying it in a way that works for the individual in front of you. Thinking of EBP as a funnel rather than a balance helps clarify that process. It shifts the goal from finding the “perfect” treatment to finding the most appropriate one for that person, at that time.
References:
Meira, E. Understanding evidence-based medicine using a funnel analogy. SportRxiv, 10, December 2020.
When is Movement “Too Much” or “Not Enough”?
In rehab, we often label movement as “too much” or “not enough”, but how do we actually know when that’s true and relevant? If you’ve ever had an injury assessment, you might have heard terms like “over-pronation” or “under-pronation.” Maybe you have too much knee valgus when you squat, your low back is hypo-mobile, your pelvis is out of alignment, or maybe it’s poor posture. The problem with many of these descriptors is that they’re largely subjective - no therapist can actually measure joint movement simply by watching you. These terms are often used to explain pain or injury, but the relationship between movement and pain is far less clear than many people assume.
In rehab, we often label movement as “too much” or “not enough”, but how do we actually know when that’s true and relevant? If you’ve ever had an injury assessment, you might have heard terms like “over-pronation” or “under-pronation.” Maybe you have too much knee valgus when you squat, your low back is hypo-mobile, your pelvis is out of alignment, or maybe it’s poor posture. The problem with many of these descriptors is that they’re largely subjective - no therapist can actually measure joint movement simply by watching you. These terms are often used to explain pain or injury, but the relationship between movement and pain is far less clear than many people assume.
Much of this comes from the concept of an “ideal.” Ideal technique, ideal posture, ideal mechanics. Anything different gets labelled “dysfunction”. The implication is that every person should move a certain way, and if you don’t move in this “optimal” way, something must be wrong and needs fixing. These explanations are often used to justify specific corrective exercises. But this approach is overly simplistic and ignores the natural variability in human bodies and pain experiences. There is certainly more discussion to be had around movement when it comes to performance — efficiency, skill, and sport-specific technique — but here we’re focusing on injury and pain.
Even if we did hook someone up to a biomechanical analysis system and measure joint angles during movement, the question still remains: when does movement become too much or not enough? Textbooks provide average ranges of motion for joints, but that’s exactly what they are — averages. What we don’t have are clear standards for when variation becomes a problem. At extreme ranges there would probably be agreement that someone has “poor posture.” But posture exists on a spectrum. At what point does it actually become “poor”? And even then, we still have several steps before confidently saying that over-pronation is the cause of your foot pain and must be corrected for you to recover.
How Are Movement Dysfunctions Measured?
Often, we simply use our eyes when assessing how someone moves. I’m certainly guilty of this. It’s jokingly call it the “vomit test”: if watching someone move makes me want to vomit, I’ll take note. Very objective and scientific (sarcasm). In reality, this is more about noticing large movement differences rather than tiny variations. There are objective tools that can improve accuracy — a goniometer to measure joint angles, a dynamometer to measure force, or slow-motion video. But even with objective data, we still face the same question: how much is too much? We simply don’t have reliable, consistent data showing that a specific angle — say 25° — suddenly becomes “over-pronation.”
Do These Movements Dysfunctions Actually Cause Pain?
Many biomechanical explanations follow a common-sense logic. It seems reasonable that there would be an ideal way to move, and any deviation would be less ideal. It also seems reasonable that someone’s flat foot might contribute to pain while running because of increased stress on the bottom of the foot. These explanations pass the common-sense “sniff test,” which is likely why they persist. But plausible explanations are not always accurate, especially when dealing with complex human systems.
Do People With Pain Actually Show These Dysfunctions?
This is where things become less clear. Research often contradicts what seems intuitive. For example, it seems logical that poor posture would lead to back pain. But we see people with poor posture who have no pain, and others with excellent posture who do have pain. Sometimes the relationship may even run the other direction - pain can influence posture. Someone with disc-related back pain may shift their torso sideways simply because it reduces symptoms. In that case, the posture isn’t the cause of pain but a response to it.
Can These Movement Patterns Actually Be Changed?
Many treatment approaches focus on correcting these perceived dysfunctions through specific exercises. These are typically highly cued, low-load “motor control” exercises designed to help you feel and control certain movements or positions. The idea is that repeating these exercises will eventually correct the dysfunction and resolve the pain. But research often shows that these movement patterns don’t actually change — even when pain improves. So what caused the improvement? Was it the exercises themselves? General physical activity? Natural recovery? Expectations about the treatment? Pain and movement are complex systems, and rarely explained by a single factor.
Do You Need to Change Your Movement to Get Out of Pain?
This is the real question, and the heart of my position. Humans are highly individual in how they move. We naturally develop movement patterns that feel comfortable and efficient for us. Do we really want to change what is natural for every individual? Usain Bolt, the fastest man in the world, has noticeable scoliosis. Through training, he has adapted to it while setting world records in the 100 metres. If we tried to “correct” his scoliosis, would that make him faster — or slower? Many elite marathon runners display foot mechanics that many clinicians would label over-pronation (in fairness, I probably would too). Yet they perform at the highest level. Would it make sense to change the very mechanics that got them there? This situation occurs frequently in rehab. A runner develops knee pain, completes rehabilitation, and their pain resolves — yet they continue running exactly the same way as before. If they entered and exited pain without changing their running mechanics, can we really blame the mechanics? Sometimes we do temporarily change movement patterns, but not because the movement itself is faulty. Instead, the goal is to unload a sensitive structure. Once symptoms settle, we gradually build capacity again.
This is why I’m skeptical of the over/under and hyper/hypo labels for posture and movement. Often the measurement isn’t reliable, the link to pain isn’t clear and many of these “dysfunctions” either can’t be changed or don’t need to change for pain to improve. I understand the appeal of this idea: fix this dysfunction and you’ll fix your pain. It’s simple and reassuring, but it can also create misleading narratives. People start to believe their bodies are fragile. They worry that moving the wrong way will cause injury. Small aches lead to fear, avoidance, or compulsive corrective exercises. Ironically, letting go of the need to fix every perceived dysfunction often opens more options in rehab. It shifts the focus towards building strength, tolerance, and confidence in movement, rather than chasing perfect mechanics. This is usually what gets people back to doing what they enjoy.
(Credit goes to Greg Lehman’s Reconciling Biomechanics with Pain Science for the inspiration for this blog and this thought process that helped me develop into the therapist I am today.)
"What a Difference Some Exercise and Time Makes”
This recent case highlights how patient education, realistic expectations, and a clear rehab plan can shape recovery.
This recent case highlights how patient education, realistic expectations, and a clear rehab plan can shape recovery.
A 69-year-old retired male had been running casually for over 10 years, typically 6–10km every other day from spring through fall. In early November, he felt some lower right glute pain during a run but was able to finish. After resting a week, he attempted another run and developed sharper pain around 2km in, forcing him to walk home. Since then, he had been resting and stretching. He noticed his flexibility improved, but the pain persisted — particularly with a few attempts at running. In January, after a delayed four-hour flight, he developed more significant pain down the back of his right leg. Sitting aggravated it, and a long Christmas dinner was his worst day. The leg pain, and how long it was taking to improve despite doing nothing to aggravate it, were what concerned him the most.
Patient Education
Early on, the priority was providing an explanation for his leg pain. Clinically, this presentation was consistent with proximal hamstring tendinopathy: common in runners and often aggravated by sitting pressure. We discussed the possibility of an initial gluteal strain but questioned it given the relatively low-load nature of distance running. The key message wasn’t obsessing over the perfect label. It was explaining: why sitting hurt, why symptoms evolved, why rest alone hadn’t solved it, what tendons actually need to improve, and how we could tackle both pain points. That led directly into expectations.
Setting Expectations
He was used to minor “niggles” resolving in 1–2 weeks. The concern was this felt different; even different from his prolonged ITB pain years ago, which left him frustrated by unclear explanations and slow progress. With spring approaching, he felt pressure for this to “heal now.” We discussed that tendinopathies are notorious for slower timelines — often 2–8 months depending on duration and loading consistency. This timeframe is not because something is severely damaged, but because tendons adapt gradually. He didn’t love that timeline, but having one was better than uncertainty. Understanding what is typical often reduces anxiety more than promising quick fixes that don’t pan out.
Proper Loading
During his rest period, he had mainly been stretching. Stretching can feel good and reduce pain temporarily, but tendons respond best to progressive resistance training. We introduced three primary exercises: hip thrusts, Romanian deadlifts (RDLs), and floor-sliding hamstring curls. The focus was on progressive loading of the proximal hamstring and glute through hip extension and knee flexion. We also discussed getting creative with loading, since his available weights were light. With hip hinges especially, most people can tolerate going relatively heavy. We kept stretching in the plan since he found it helpful and it wasn’t interfering with recovery, but strengthening became the priority.
Two Weeks Later
At follow-up, the first thing he said was: “What a difference some exercise and time makes.” He reported several days completely free of leg pain; the glute discomfort was still present but improved. He also noticed continued flexibility gains despite doing less static stretching and more strengthening. We progressed his RDL to a split-stance variation to increase single-leg loading without needing heavier weights. Next steps will include further progression and building toward a structured return-to-run plan.
Why This Case Matters
Despite being a running-related injury, improvement didn’t require anything fancy. It required a clear explanation, realistic expectations and progressive loading. Education reduced uncertainty, expectations reduced anxiety, and loading gave the tissue a reason to adapt. This wasn’t about chasing symptoms; it was about rebuilding capacity. It was about restoring capacity. Nothing flashy. Just the sound rehab principles of clear communication, calming things down and building them back up.
When “Abnormal” Is Normal: Rethinking Rotator Cuff Tears and MRI Findings
A new research paper is making the rounds, and while the headline numbers may surprise the general public, for clinicians it’s another reminder of something we’ve been seeing for years: age-related changes on imaging are incredibly common.
A new research paper is making the rounds, and while the headline numbers may surprise the general public, for clinicians it’s another reminder of something we’ve been seeing for years: age-related changes on imaging are incredibly common.
Ibounig and colleagues performed MRIs on both shoulders of 602 Finnish adults aged 41-76 to examine how common rotator cuff “abnormalities" were - defined as tendinopathy, partial-thickness tears (PTRCTs) or full-thickness tears (FTRCTs). What they found was:
592 of the 602 participants (98.8%) had abnormalities
25% had tendinopathy, 62% had PTRCTs, 11% had FTRCTs
Prevalence and severity increased with age, as tendinopathy was more common in those 41-54 and tears more common in those 55 and older
Abnormalities were present in 96.6% of asymptomatic shoulders and 98% in symptomatic shoulders.
Overall, nearly everyone over 40 had something show up on their MRI, regardless of whether they had pain. This may sound dramatic, but it is consistent with previous research. What this paper reinforces is not that shoulders can “fall apart”, but that structural changes are a normal part of aging.
Takeaway #1: What Does “Abnormal” Mean?
If 98.8% of people have something, can we really call it abnormal? By definition, abnormal means no normal (duh), unusual or deviating from the norm. But when almost everyone over 40 shows these findings, wouldn’t that just be normal? We could argue that a “normal” shoulder should be free of degeneration or tears, but that ignores biology. Just like skin wrinkles and hair turns grey, rotator cuff tissue changes with age. We’ve traditionally labelled these findings as degeneration, defects or lesions, but when changes are this common (and often painless), maybe our language needs updating.
Takeaway #2: Pain is Not the Same as Imaging
One of the most important findings in this paper is the lack of difference between painful and non-painful shoulders, with those two groups having close to the same prevalence of abnormalities. It makes sense to assume that a tear must hurt (especially a FTRCT), but this ignores the complexity of pain. Tissue quality is only one piece of the puzzle; psychological, social and even other biological factors all influence whether someone experiences pain and how intense that pain is. An MRI simply shows structure. It does not show pain, nor does it show when the tear occurred, if it’s relevant, how strong the shoulder is or how confident someone is in using their shoulder. As the authors note, “While we cannot dismiss the possibility that some rotator cuff tears may contribute to shoulder symptoms… we are currently unable to distinguish clinically meaningful MRI abnormalities from incidental findings.” Imaging can support a diagnosis (especially in cases of clear acute trauma or significant strength or functional loss) but it cannot be the sole explanation for pain.
Why This Matters
For clinicians, this paper reinforces the need to be thoughtful with our language. Terms like “degeneration” or “defect” imply something is broken and needs fixing. But many of these findings are common age-related changes, not structural catastrophes. For patients, this can be reassuring. If you’ve been told you have a tear - especially if. you don’t even have pain - this paper suggests your shoulder may be far more normal than you were led to believe. Even if you do have pain, this doesn’t automatically mean your shoulder is fragile damaged or destined for surgery.
Age-related changes are not exclusive to the shoulder. We see similar patterns in the spine and knee: structural changes increase with age, but the link to pain is inconsistent. You are not your imaging. The human body is adaptable and resilient. The goal isn’t to fix every MRI finding, but to build strength, restore capacity and help you reclaim confidence in your movement.
Ibounig T, Jarvinen TL, Raatikainen S, Harkanen T, Sillanpaa N, Bensch F, et al. Incidental rotator cuff abnormalities on magnetic resonance imaging. JAMA Intern Med. 2026.
If You Throw, You Need A Different Kind of Rehab
Baseball and softball are growing in numbers and visibility in Ireland, especially at the recreational level. Injuries can and still do occur, but sports medicine is understandably built around hurling, Gaelic football and rugby. Throwing in baseball and softball is different. The forces are different. The long-term adaptations are different. Therefore the rehab has to be different too. If you throw, you need someone who understands throwers. Treating a thrower like a general shoulder is misguided.
Baseball and softball are growing in numbers and visibility in Ireland, especially at the recreational level. Injuries can and still do occur, but sports medicine is understandably built around hurling, Gaelic football and rugby. Throwing in baseball and softball is different. The forces are different. The long-term adaptations are different. Therefore the rehab has to be different too. If you throw, you need someone who understands throwers. Treating a thrower like a general shoulder is misguided.
The Hidden Forces of Throwing
Throwing a baseball is one of the most stressful movements in sport, especially for pitchers. At maximum layback, the elbow experiences roughly 60lbs of torque (the equivalent of five bowling balls pulling down on it). At ball release, the shoulder experiences a distractive force of about 1.2 times bodyweight, meaning the joint is resisting forces that are actively trying to pull it apart. All of this happens in less than a second, with the arm rotating at nearly 7,000° per second. These aren’t normal gym demands. Throwing places extreme stress on the shoulder and elbow at speeds and forces most rehab programs never prepare you for. Bands and light dumbbells might help early on, but if rehab never progresses to heavy strength work, eccentrics, plyometrics, medicine balls, and actual throwing, you’re not preparing for competitive throwing. If rehab doesn’t build you for the demands of throwing, it isn’t baseball rehab.
When Abnormal is Actually Normal
Because of the extreme forces involved in throwing, pitchers develop adaptations that don’t look “normal”, and they aren’t supposed to. The problem is that these adaptations are often treated as something to correct. A throwing shoulder is not a general population shoulder.
One of the best examples is humeral retroversion. After years of throwing, especially during youth development, the humerus gradually twists outward. This increases external rotation (ER) and decreases internal rotation (IR). This shift isn’t a flaw. More ER generally means more velocity. It also allows pitchers to achieve layback without over-stressing the front of the shoulder, because part of that motion is coming from bone structure and not just soft tissue laxity. But here’s where misunderstandings happen. A player presents with shoulder pain, IR looks limited, it gets labeled as GIRD (glenohumeral internal rotation deficit), and posterior capsule stretches are prescribed to “restore” the lost IR. Yet when both arms are measured properly, the total arc of motion in the throwing arm should be within about 5–10° of the non-throwing arm. If total arc is preserved, that “loss” of IR is just humeral retroversion — a normal and beneficial adaptation. Trying to aggressively correct that can mean altering the very adaptation that helps performance. This is why comparing a thrower’s shoulder to population norms can be misleading.
Labral findings are another example. Many throwers show labral changes on imaging due to the repetitive “peel-back mechanism” when throwing. However, many remain asymptomatic. Imaging findings alone do not equal dysfunction, especially in throwers. Treating the scan instead of the athlete is misguided. In throwers, the question isn’t “does this look normal?” It’s “is this functional and resilient for the demands of throwing?”
Asymmetry is a Feature, Not a Flaw
Baseball is inherently one-sided. You throw with one arm, you rotate in one direction, you load the same hip and shoulder, over and over again. The body adapts to this repeated stress - that’s the S.A.I.D. principle at work. Over time, throwers become structurally and functionally asymmetrical because the sport demands it. Rehab and strength training often aim for symmetry. Restoring baseline strength after injury is important but it’s in reference to the uninjured side. Perfect symmetry isn’t the goal in baseball; the goal is resilience within the asymmetry. A thrower doesn’t need to look balanced — they need to tolerate the demands of their position. In baseball, functional asymmetry is normal.
Return-to-Throwing is a Skill
Developing a return-to-throwing plan for a baseball or softball player is complex. Most interval throwing programs (ITPs) progress using distance (as a proxy for intensity) and number of throws (volume). This seems logical, but in reality, it’s far messier. Without wearable technology to measure elbow stress, or even a radar gun to monitor velocity, maintaining consistent intensity from session to session is difficult. Distance alone does not equal force as there is no perfectly linear relationship between how far you throw and how much stress is placed on the arm. Two pitchers who both throw 90mph do not necessarily place the same amount of stress on their arm either. Differences in mechanics, timing, strength, and body structure all change the equation. You can throw a short distance with maximal effort. You can throw farther with less effort. And that’s before we even introduce tools like weighted balls, long toss, and pulldowns. These methods may be effective for building arm strength and velocity because they intentionally increase stress on the system to drive adaptation, but they also alter mechanics and increase load. If used incorrectly or layered into a rehab process too early, they can easily set a player back.
Returning to throwing after injury is not just about being pain-free - it’s important but not the same as being ready to throw. Readiness requires: appropriate progression, controlled volume, gradual exposure to higher intensities, adequate recovery, and mechanical awareness. Returning to throwing is a matter of exposure to stress, and if you get the stress wrong, you can experience setbacks.
Specialized, Not Standard
If throwing creates unique adaptations, then our standards for assessment must reflect that. We cannot assess or rehab a thrower’s shoulder the same way we would a non-thrower’s. In general rehab, we often use the uninvolved side as the reference, but a thrower’s dominant arm should not look like their non-dominant arm or like the general population. Throwers often need greater ER strength, specific strength ratios that differ from standard “norms”, and unique endurance demands. If we apply generic shoulder strength standards to a thrower, we risk under-preparing them for the demands of throwing or over-correcting adaptations that are actually beneficial. A thrower’s shoulder isn’t broken because it doesn’t look symmetrical or textbook-normal; it’s specialized and specialized athletes require specialized assessment.
Protecting the Developing Arm
When we think about kids, we tend to imagine they’re indestructible — flexible, resilient, and able to bounce back from anything. Kids are just as susceptible to overuse injuries as adults, but the injuries look different. A common example is Little League Elbow (LLE). This is irritation of the growth plate on the inside of the elbow caused by repetitive throwing stress. In young athletes, the growth plate is the weak link in the arm. That’s why we don’t commonly see 10–14 year olds tearing their ulnar collateral ligament (UCL). The growth plate fails first. Once that plate closes (typically 15–17 years old) the weak link shifts and now the UCL becomes the structure at risk. The stress doesn’t change but rather the tissue that absorbs it does.
LLE is, at its core, an overuse injury and it reflects a broader issue in youth sports: early specialization and year-round competition. The baseball culture of today with travel teams, showcases, and constant exposure can quietly accumulate thousands of throws on a developing arm. This matters, especially when recovery, strength development, and overall athletic diversity are limited. Protecting young throwers isn’t about shutting them down. It’s about: managing throwing volume, respecting recovery, prioritizing long-term development over short-term exposure, and educating coaches and parents on how the throwing arm actually develops. Understanding the throwing shoulder and elbow isn’t just about rehab - it’s about prevention and giving young athletes the chance to keep playing for years to come.
Throwing is what makes baseball and softball unique and it’s also what makes players different to rehab. As the sports continue to grow in Ireland — in numbers, competition, and visibility — the need for informed, sport-specific injury management grows with them. Throwers cannot be assessed, progressed, or returned to play using generic shoulder guidelines. If you throw, you need someone who understands throwers. My role isn’t just to reduce your pain. It’s to understand the demands of your position, your schedule, and your long-term goals. It’s to manage load, guide progression, and prepare your arm for the realities of competition. It’s to return you to the field with confidence, not just clearance, because being pain-free isn’t the same as being ready.
The Activity is the Rehab
The purpose of a rehab plan shouldn't be just to get you out of pain and heal the injured area, but to prepare you to return to your sport or activity feeling confident and ready to go. This is something that is often missing from rehab.
The purpose of a rehab plan shouldn't be just to get you out of pain and heal the injured area, but to prepare you to return to your sport or activity feeling confident and ready to go. This is something that is often missing from rehab. I’ve worked with countless patients who either completed rehab but didn’t feel they were ready for sports again, or who never progressed beyond simple rehab exercises and were still dealing with their injury. A great way to bridge the gap between rehab and a return to your activity is to incorporate the activity into the rehab; the activity is the rehab.
When and how we do this depends on factors like the type of injury, how long it has been present, the level of pain or sensitivity, and the sport itself. For example, for a runner who just sprained their ankle, we’re going to manage their pain and swelling and work on range of motion and strength before we worry about running again. But for a runner dealing with a hamstring tendinopathy, we may still be able to incorporate some running with modified parameters into their rehab if they can tolerate it.
The reason we need to incorporate the activity into the rehab plan comes back to the S.A.I.D. principle. With continued participation in a sport, we not only develop specific adaptations to that sport, but also a level of tolerance to its demands and forces. Each sport is going to have its own unique demands on the body, and nothing can prepare you for your sport like doing the sport itself.
Looking at running again since many sports involve some form of it, each stride can result in 2-3 times a person’s body weight going through their leg at a slower pace, and up to 6-8 times body weight at faster paces. Depending on the individual, the injury and equipment available, it may be very difficult to achieve these kinds of loads with rehab and strengthening exercises alone. Simple plyometric exercises like hopping and jumping come close to reproducing these forces and can be a great introduction, but ultimately if the goal is to return to running, then at some point the body has to be exposed to running again.
It’s important not to create a false dichotomy and think that strengthening isn’t important. Strength and rehab exercises build the physical strength and power needed for the sport and support the rehab process. Sport-specific activity prepares the body for sport by reintroducing those unique demands. Likewise, it doesn’t mean we just push through pain to maintain training tolerance. A good rehab program brings the exercises and activity down to a level the person can tolerate, and builds up from there.
Incorporating the sport into the rehab can also be great from a psychological aspect. Having to stop doing an activity you enjoy can make recovery seem more unattainable as thoughts of never being able to return may creep in. Finding ways to incorporate some degree of the sport can help you feel like a return is possible and provide encouragement along the way.
Rehab shouldn’t end when the pain fades; it should end when you feel prepared, and nothing can prepare you for your sport like doing the sport itself. Modify it to what you can tolerate, and build from there. That’s how you bridge that gap physically and mentally.
Rest Is Not Lazy
Last week, I explained why rest alone is not rehab. This week, I want to address the other side of that conversation: resting isn’t being lazy. While we often feel the need to be actively doing something throughout our entire rehab, rest can be a valuable tool when used appropriately. Rest isn’t the opposite of rehab, but rather a part of it.
Last week, I explained why rest alone is not rehab. This week, I want to address the other side of that conversation: resting isn’t being lazy. While we often feel the need to be actively doing something throughout our entire rehab, rest can be a valuable tool when used appropriately. Rest isn’t the opposite of rehab, but rather a part of it.
Inflammation: Helpful Until It Isn’t
Rest is most important in the first few days following an acute injury. This phase, known as the inflammatory stage of healing, is an immune response that helps clean up the injured area and set the stage for recovery. Inflammation isn’t a bad thing — it’s necessary. However, it’s also typically the most painful phase, which serves as a reminder that the tissue is vulnerable. Ignoring this phase can lead to further injury or a larger inflammatory response, both of which can slow recovery. Gentle range-of-motion movements are often appropriate here, but rest at this stage is about respecting the healing process, not pushing through it.
Stress Builds, Rest Rebuilds
When we train in the gym, we don’t usually work the same muscle group hard on consecutive days. The time in between allows the body to recover and adapt. Rehab works the same way. Rehab exercises provide the stimulus, but the body responds and heals during rest. Without enough time to recover, even well-designed rehab exercises can become another stressor rather than a benefit.
Progress Loves Patience
Many injuries are related to doing too much, too soon, or too often without enough recovery. Overuse injuries aren’t usually caused by a single mistake, but by a gradual mismatch between training demands and recovery. Building rest into your training helps manage this. Setbacks or flare-ups aren’t failures — they’re often just load miscalculations that signal the body wasn’t fully prepared for the demands placed on it.
More Than Just the Tissue
Injury is never just a physical issue. The same biopsychosocial factors that influence injury also influence pain and recovery. Your body is constantly balancing training, work stress, sleep, nutrition, and social pressures. When rest is consistently ignored, fatigue builds and tolerance for both activity and healing drops. Strategic rest helps calm the system as a whole and not just the injured tissue.
The goal of rest isn’t to slow you down — it’s to set you up for future training. Rest is when the body repairs itself after you’ve given it a reason to adapt. Smart rehab is knowing when to push and when to pause. Rest alone isn’t rehab, but rehab without rest doesn’t work either.